Retired nurse gives high praise to cardiac care staff
Anne Marcotte was not used to being on the other end of a stethoscope.
The 75-year-old Topeka resident spent most of her career as a registered nurse in California hospitals before retiring after 52 years.
“When I was a brand new cardiac care nurse in the 1980s,” Anne said, “our hospital would do five to six coronary bypasses a day. I quickly became familiar with the procedure, from a nurse’s viewpoint, but I didn’t really know how to be a cardiac patient.”
As she was preparing to retire and move to Topeka, Anne started experiencing bouts of shortness of breath, so her doctor ordered a stress test. During the test, the participant usually walks on a treadmill or rides a stationary bike. The staff constantly monitors the participant’s heart to see how well it performs during exercise.
“I failed miserably,” Anne said. “The doctor said he wanted to do a cardiac catheterization right away to see if there were any blocked arteries. But since I was leaving California, I didn’t want to start the process until I reached Kansas. Once I got to Topeka, I made an appointment with Dr. Arnold Graham, and he's been taking care of me ever since.”
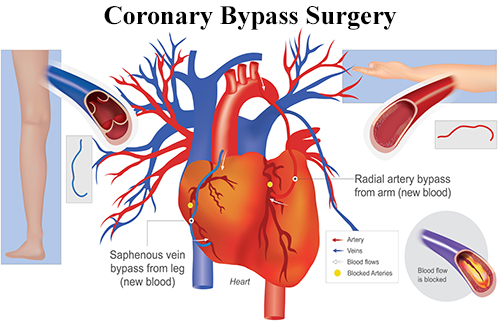
Coronary Bypass Surgery
Anne liked Dr. Graham’s style of care, as he was diligent in collecting data before making a diagnosis.
“We’ll keep an eye on you,” said Anne, recalling Dr. Graham’s words. “So over the next five to six years, I completed a regular schedule of stress tests to keep track of how well my heart was working. I also tried to stay active by walking my dog and going to the gym with my niece three times a week. Those activities helped me lose some weight, which was good for my heart and Type 2 diabetes.”
 Then in October 2022, Anne started having chest pains when she walked more than a short distance. That’s when Dr. Graham ordered a cardiac catheterization and found that Anne had blockages in three of the four major arteries. After that diagnosis, she was quickly scheduled to have triple bypass surgery at The University of Kansas Health System St. Francis Campus.
Then in October 2022, Anne started having chest pains when she walked more than a short distance. That’s when Dr. Graham ordered a cardiac catheterization and found that Anne had blockages in three of the four major arteries. After that diagnosis, she was quickly scheduled to have triple bypass surgery at The University of Kansas Health System St. Francis Campus.
Coronary bypass surgery creates a new path for blood to flow around a blocked artery in the heart. In Anne’s case, three new paths would need to be created. For each new path, a healthy blood vessel is taken from the chest or leg area and is connected above and below the blocked artery. This restores blood flow to the heart.
Following the surgery, Anne stayed in the Intensive Care Unit for three days while the nurses closely monitored her blood pressure and other vital signs. She was then transferred to a room on the telemetry floor where she was also closely monitored until she was discharged to go home.
Cardiac Rehabilitation
Less than a month after her surgery, Anne started her cardiac rehabilitation program at the health system’s St. Francis Campus, near Dr. Graham’s office.
“It was very convenient,” said Anne. “The first day I went there, my heart rate was really slow because of the medications I was on. The rehab staff was able to go down the hall and talk to Dr. Graham about my condition, which led to a change in the way the medication is given. That was great patient care!”
Anne now works out three days while connected to telemetry equipment to monitor her vital signs. This phase of the program lasts 12 weeks.
“I walk on the treadmill up to eight minutes and then I do eight minutes on the seated stair stepper,” Anne explained. “You know, it's hard to get back into the swing of things, but eight minutes is pretty good. On the days that I don’t go the workout sessions, I walk around my neighborhood,” she said.
She would like to build up the strength to walk her dog, Livvie, at the dog park. “She's kind of headstrong and likes to pull away, which is not good for my sternum – the site of my surgery.”
When the weather is nice, Anne will often work outside, pulling weeds in her garden.
“I was lucky to buy a house from an owner who had planted thousands of bulbs, including irises and tulips. I also added daylilies and roses, so there are lots of colors in my yards, which I love. The lilac bush in my front yard is blooming now,” she said.
In her quest to lose more weight, Anne follows a heart-healthy diet to help manage Type 2 diabetes. “The biggest thing is decreasing the amount of salt in my diet. It’s hard to do sometimes, but I have to do it. This past week, I lost two and a half pounds, so the diet and exercise are working. I am thrilled!”
Strong Recommendations
Through it all, Anne had high praise for the cardiac staff at The University of Kansas Health System St. Francis Campus.
“I’ve got to say, I was just blown away by the staff who work in the ICU, on the Telemetry floor and in the rehabilitation center,” Anne explained.
“Every single nurse and staff member who cared for me was upbeat, positive, eminently capable and appeared to love working there. Their demeanor was obviously a credit to their caring nature and their professionalism. I had an outstanding stay and would highly recommend them to any and all friends and family.”
“You guys have got it going on.”
To learn more about our cardiac care services and healthcare providers, visit the department’s web page.