Joint Replacement in Northeast Kansas
Living with pain in your joints can be challenging. If you are experiencing pain in your knee, hip or shoulder that is affecting your daily life, it may be time to see an orthopedic specialist to talk about joint replacement surgery.
Joint replacement can be a life-changing procedure for those who have been struggling with chronic joint pain. Imagine being able to live your life without pain, sleep better, regain your independence and get back to doing the things you enjoy. A joint replacement can get you there.
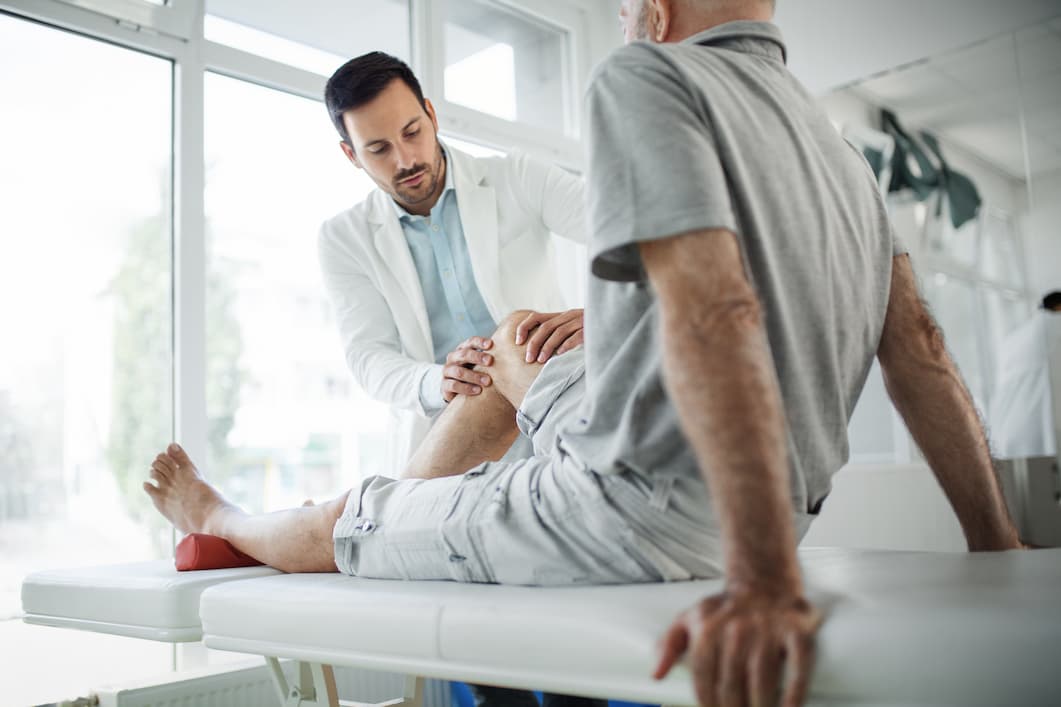

Joint replacement is a safe and effective procedure that can improve joint function, reduce pain and enhance quality of life. More than one million joint replacements are performed in the U.S. each year, and a hip or knee replacement done today can last for 20 or more years.
The providers of Orthopedics and Sports Medicine at The University of Kansas Health System St. Francis Campus stand at the forefront of surgical treatment for bone and joint problems. Our advanced technologies allow for quicker recovery and less pain than joint replacements from just a few years ago. That means we can get you back to your life faster.
We believe that effective joint replacement requires a combination of surgical expertise and collaboration among primary care physicians, specialists and rehabilitation experts. This approach led to the development of the Joint Replacement Center at The University of Kansas Health System St. Francis Campus. The center is a dedicated inpatient department within the hospital that utilizes preoperative education, highly specialized staff, group physical therapy and other special amenities to enhance your recovery, reduce costs and shorten your length of stay. Our team has one goal: to help you live your best life.
Take the first step towards a pain-free, active lifestyle by scheduling an appointment with one of our experienced orthopedic experts. Call 785-233-7491 today.
Frequently Asked Questions About Joint Surgery
What causes joint pain?
Our joints are in constant movement. When a joint starts to wear out, the cartilage (or cushioning) around the joint breaks down, causing bones to rub together. Advanced and end-stage joint disease can be caused by:
- Osteoarthritis
- Rheumatoid arthritis
- Other inflammatory joint problems
- Previous joint injuries
- Joint infections
- Other rare conditions that cause chronic joint pain
What is joint replacement?
A total joint replacement (also known as arthroplasty) is a surgical procedure performed by an orthopedic surgeon. During the procedure, the arthritic or damaged areas of the joint are removed and replaced with a metal or plastic device. This device is designed to replicate the movement of a normal, healthy joint. Hip and knee replacements are the most common joint replacements, but replacement surgery can be performed on other joints, such as the ankle, wrist, shoulder and elbow.
Who is a candidate for joint replacement?
The first step for a joint replacement procedure is to meet with an orthopedic doctor. They can use diagnostic imaging and a physical examination to diagnose and determine if a joint replacement is right for you.
Depending on your results, an orthopedic specialist may recommend joint replacement surgery if:
- You suffer from limited mobility, swelling or stiffness that severely limits your daily activities and quality of life.
- You’ve already tried other non-surgical joint pain treatments, such as exercise modifications, physical therapy, anti-inflammatory medications, injections and braces.
- You continue to experience a decline in function and disabling pain.
What are the latest technologies available for joint replacement procedures?
Our surgeons use many of the latest treatments and newest technologies to perform less-invasive procedures.
Mako SmartRobotics™ is an innovative solution for many suffering from painful arthritis of the knee or hip. Mako uses 3D CT-based planning software so your surgeon can know more about your specific anatomy to create a personalized joint replacement surgical plan. This 3D model is used to pre-plan and assist your surgeon in performing your joint replacement.
The anterior approach to hip replacement, or total hip arthroplasty, allows doctors to perform a hip replacement surgery with a minimally invasive technique, using a smaller incision on the front (anterior) of the hip rather than the back or side. This generally results in less trauma to the tissue under the skin, which means less pain and a faster recovery.
What is recovery like after joint replacement and how soon can I return to normal daily activities?
Recovery varies from patient to patient and is dependent on a number of factors including the type of procedure performed and the patient’s age, weight and activity level. Some patients who receive joint replacement are able to return home the same day as surgery while others may require a short overnight stay in the hospital. It is typically expected that the patient is able to independently get in and out of bed, get dressed and use the toilet at the time of discharge.
Many joint replacement patients are routinely standing and walking within a day or two of surgery with the aid of an assistive device such as a cane, walker or crutches. Some patients are even walking the same day as surgery. Most patients are able to resume driving within 2-8 weeks once they have discontinued use of opioid pain medications and have received approval from their doctor. The timeline for a patient to return to work will vary. Someone with a sedentary job may be able to return to work within a few weeks, while someone with a more physically demanding job will require a longer recovery before returning to work.
Every person’s anatomy and situation are unique, so it’s important to discuss your specific recovery timeline with your orthopedic surgeon.
What is the first step in the joint replacement surgery process?
To determine if joint replacement is right for you, make an appointment with one of our orthopedic specialists at 785-233-7491. During your appointment, we will perform a full evaluation to determine the best treatment option for you.
Mako Smartrobotics™ Can Help Relieve Arthritis Pain
If you’re one of the millions of Americans suffering from knee pain or hip pain caused by arthritis or an injury, and you haven’t experienced relief with traditional treatment options, Mako Robotic-Arm Assisted Surgery may be right for you.
Mako SmartRobotics™ is an innovative joint replacement technology for many who are suffering from painful arthritis. Mako allows your surgeon to create a customized surgical plan unique to your individual anatomy. Before surgery, a CT scan of the diseased joint is taken and used to create a 3D model of your joint. This 3D model is then used to pre-plan and assist in performing your joint replacement.
During the procedure, your surgeon guides Mako’s robotic arm within the predefined area. Mako technology prevents your surgeon from moving outside the boundaries defined in your surgical plan to help protect your healthy bone. Mako also allows your surgeon to make adjustments to your plan during surgery as needed. It’s important to understand that Mako does not perform surgery, make decisions on its own or move without the surgeon guiding it.
The combination of 3-D scanning and robotically guided cutting helps the physicians create a better joint than was previously possible. For the patient, surgery with the new system offers several benefits, including:
- Smaller incision
- Less scarring
- Reduced blood loss
- Shorter hospital stay
- Quicker recovery
- A more natural-feeling knee after less-invasive surgery
The Anterior Approach to Hip Surgery
Having a hip replaced can restore your quality of life, but it’s still a serious surgical procedure. Now, with the anterior hip replacement technique, qualified patients can undergo this procedure with less pain and faster recovery time and often see their range of motion return almost immediately.
This procedure allows doctors to perform hip replacement surgery with a minimally invasive technique, creating multiple benefits for the patient.
The surgery uses a smaller incision on the front (anterior) of the hip rather than the back or side, generally resulting in less trauma to the tissue under the skin.
While traditional hip replacement patients usually stay about three to five days in the hospital, those undergoing anterior hip surgery often have shorter stays – commonly one to two days.
Following the anterior approach procedure, patients usually enjoy a greater range of movement almost immediately. In most cases, patients can use their hip normally without restrictions.
As the incision is on the front of the hip, patients don’t incur the pain of sitting on the incision site. There’s also a smaller surgical scar left by the anterior approach.
Not all patients are candidates for the anterior approach. The results and recovery from hip replacement depend on a wide range of factors including age, weight and activity level. If you’re tired of living with hip pain, talk to your orthopedic surgeon about what’s best for you.
Call to schedule a consult today. 785-233-7491
Sources: The American Academy of Orthopaedic Surgeons and the American College of Rheumatology.